Cultural Sensitivity in GDS: A Global Senior Care Guide
February 20, 2026 | By Arthur Vance
Depression is a universal human experience, but it does not look the same in every corner of the world. For many seniors and their families, recognizing the signs of a mood disorder can be difficult. Is a grandmother's constant fatigue just a sign of aging, or is it something deeper? When a grandfather stops talking about his feelings, is he showing strength, or is he struggling with a silent burden? Cultural backgrounds shape how we talk about sadness, how we experience stress, and how we seek help.
How can we accurately measure mental health across different cultures? This is where the Geriatric Depression Scale (GDS) becomes an essential tool. While the science behind the scale is robust, applying it requires a deep understanding of cultural nuances. If you are a caregiver or a healthcare professional, understanding these differences is the first step toward providing better cross-cultural screening. To get started with a scientifically backed assessment, you can begin your culturally adapted GDS assessment on our platform today.
This guide explores why cultural sensitivity is vital when using the GDS. We will look at how symptoms vary globally and how digital tools can help bridge the gap between language and understanding. Our goal is to ensure that every senior, regardless of their background, receives the mental health support they deserve.

Why Cultural Context Matters in the Geriatric Depression Scale
The Geriatric Depression Scale was designed to be a simple "Yes/No" tool to identify depression in older adults. However, a "Yes" in one culture might mean something very different in another. Culture acts as a lens through which we view health. In some societies, emotional health is discussed openly. In others, it is a private matter that is rarely mentioned, even to family members.
When using the cultural geriatric depression scale approach, we must realize that language is only one part of the puzzle. The way a person perceives the questions is influenced by their upbringing, religion, and social environment. Without considering these factors, a standard screening might miss the subtle cries for help from a senior who expresses their pain differently.
Somatization: When Depression Manifests Physically
In many cultures, especially in parts of Asia, Africa, and Latin America, depression is often expressed through "somatization." This means that instead of saying "I feel sad" or "I feel hopeless," a senior might complain of physical symptoms. They may report chronic headaches, stomach pain, or persistent fatigue that has no clear medical cause.
If a caregiver only looks for "sadness," they might miss these physical indicators. The GDS is helpful because it focuses on the quality of life and energy levels rather than just "feeling blue." By using an online GDS tool, you can see how these physical and emotional questions correlate to provide a clearer picture of a person’s mental state. Understanding that "my body hurts" can sometimes mean "my heart is heavy" is a vital skill for any modern caregiver.

The Role of Stigma in Self-Reporting
Stigma remains one of the largest barriers to mental health care globally. In many communities, admitting to a mental struggle is seen as a sign of weakness or a source of shame for the entire family. This stigma can lead seniors to answer GDS questions in a way that makes them appear "fine," even when they are struggling.
For example, a question like "Do you feel that your life is empty?" might be very difficult for someone from a culture that highly values family roles. They might feel that answering "Yes" is a betrayal of their children’s efforts to care for them. Professionals must approach these questions with empathy, ensuring the senior knows the assessment is a private tool designed to help them feel better, not to judge their life choices.
GDS Cross-Cultural Validity: Adaptation Essentials
To make the GDS a truly global tool, researchers have worked hard to ensure GDS cross-cultural validity. This means checking if the test actually measures depression accurately in different populations. It involves more than just translating the words; it requires adapting the concepts to fit local realities.
A tool that works perfectly in London will require customization to work in Tokyo or Mexico City. This scientific process ensures that the results are reliable and that the "cut-off" scores (the numbers that indicate a risk of depression) are appropriate for the specific group being tested.
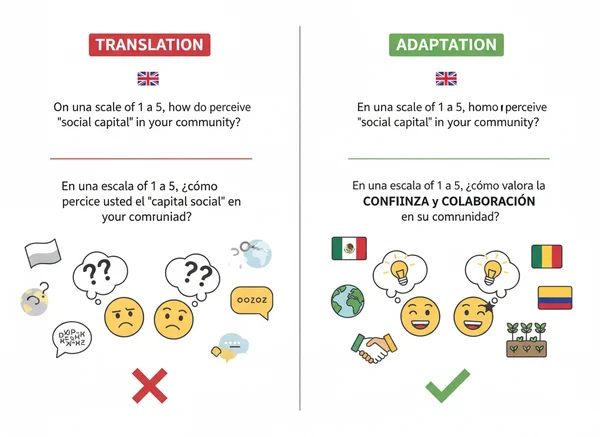
Translation vs. Adaptation: Why Words Matter
There is a major difference between a simple translation and a clinical adaptation. A literal translation might use words that sound awkward or confusing to a native speaker. For instance, the English idiom "feeling down in the dumps" does not have a direct equivalent in many languages. If translated literally, a senior might find the question strange and answer incorrectly.
True adaptation focuses on the intent of the question. Our website offers the GDS in 16 supported languages. Each version is designed to be clear and culturally appropriate. This ensures that when a user chooses their native tongue, they are seeing questions that make sense to their specific cultural experience, leading to much more accurate results.
Adjusting GDS Scoring and the GDS Short Form
Scoring is another area where culture plays a role. In clinical settings, a score of 5 or higher on the GDS-15 (also known as the GDS short form) usually suggests a risk of depression. However, research has shown that these cut-off scores require customization depending on the population.
Factors like education level, religious involvement, and even local economic conditions can influence GDS scoring outcomes. For example, in some cultures where modest or "humble" self-reporting is the norm, even a slightly elevated score might be a significant warning sign. Professionals using the GDS should always look at the person as an individual within their cultural context, rather than just looking at a number on a page.
Best Practices for Localized Depression Screening
When you are conducting a localized depression screening, the environment and the method of delivery are just as important as the questions themselves. Whether you are a family member helping a parent or a nurse in a clinic, following these best practices can improve the accuracy of the GDS.
The goal is to move from a "test" atmosphere to a "conversation" atmosphere. When a senior feels safe and understood, they are much more likely to provide honest answers that reflect their true well-being.
Creating a Safe Space for Assessment
Privacy is the foundation of a good assessment. Many seniors feel uncomfortable talking about their moods in front of other family members. They might worry about being a burden or causing worry. Whenever possible, allow the senior to complete the GDS in a quiet, private space.
Explain that the GDS is a routine part of staying healthy, similar to checking blood pressure. Use a tone that is warm, patient, and non-judgmental. If they struggle with a question, don't rush them. Let them explain their thoughts. This supportive environment reduces the fear of stigma and encourages more accurate self-reporting.
Leveraging Digital Tools for Accessibility
Digital platforms have revolutionized how we handle senior mental health. For many, an online tool is less intimidating than a formal clinical interview. An online GDS test allows users to take the assessment at their own pace, in the comfort of their home.
Our platform offers several features to help with accessibility:
- Multiple Languages: Easily switch between 16 languages to find the one the senior is most comfortable with.
- Simple Interface: Large buttons and clear "Yes/No" options designed specifically for older users.
- AI Analysis: After the test, you can choose an AI-driven report that helps interpret the score based on modern clinical insights.
- Instant Results: No waiting for a manual calculation; get a clear indication of the severity immediately.
By using these digital tools, caregivers can provide a professional level of screening without the stress of a high-pressure medical environment.
Bridging the Gap in Senior Mental Health
Cultural awareness bridges gaps in senior mental health support. By adapting tools like the GDS to honor diverse backgrounds, we show respect for each individual's life story. The Geriatric Depression Scale is a powerful ally in this mission, but it is most effective when used with cultural sensitivity.
By understanding somatization, addressing stigma, and using properly adapted tools, we can ensure that no senior has to suffer in silence. We invite you to use our free online tool to begin this journey. Whether you are a healthcare professional looking for a reliable screening method or a family member concerned about a loved one, our platform is here to provide clarity and support. Together, we can promote early detection and improve the quality of life for seniors around the world.
Frequently Asked Questions About Cultural GDS Usage
Is the Geriatric Depression Scale valid for non-English speakers?
Yes, the GDS has been extensively studied and validated in dozens of languages. However, it is important to use a version that has been professionally adapted rather than a simple word-for-word translation. Our site provides 16 validated versions to ensure accuracy for global users.
How does culture affect depression screening scores?
Culture influences how people express distress. Some cultures may report more physical symptoms, while others might "under-report" feelings of sadness due to social stigma. This means that a score should always be interpreted by looking at the person's cultural background and current life situation.
What is the difference between GDS translation and adaptation?
Translation is simply changing words from one language to another. Adaptation involves adjusting the concepts and idioms so they make sense in a local cultural context. Adaptation ensures that the GDS cross-cultural validity remains high, making the test more reliable for diverse populations.
Can I use the GDS for seniors with dementia?
The GDS is most accurate for seniors with mild to moderate cognitive impairment. For those with severe dementia, the "Yes/No" format may become difficult to follow. In such cases, other observational tools may be needed. For those in the early stages of memory loss, you can begin your culturally adapted GDS assessment to see if it is a helpful tool for your specific needs.